Pain “down there” rarely shows up on lists of chronic pain types or illustrations of the body. Social taboos keep us from openly talking about genital pain, especially if it affects sexual function. We don’t tend to think about pelvic pain all that much—unless we have it. Then we think about it a lot.

Twenty years ago, I cured myself of vulvovaginal pain. I never looked back; it had been my life’s best-kept secret.
Recently, life gave me a reason to re-examine this experience and I became curious to know exactly what I had worked out for myself all those years ago. What was that pain, and how had I fixed it?
Figuring that out became somewhat of an obsession, therapeutically speaking, and that’s when I learned that millions of women, worldwide, still suffer in silence with vulvovaginal pain.
Pain in the Vulva and Vagina is Common (so why don’t we talk about it?)
Vulvovaginal pain feels like a sharp cutting or intense burning sensation around the entrance to the vagina. Vulvodynia and vaginismus are the two most common types of “medically unexplained“ vulva pain, and they’re surprisingly more common than you might think. You’d never know it, though. Chances are, if you have vulvovaginal pain, you have not disclosed it to anyone except your partner, and you’ll see multiple doctors before you even get a diagnosis—if you ever reach out for help at all.
Although boundaries between the two conditions are not entirely clear (research is relatively new and conflicted), vaginismus is commonly described as a muscle spasm that closes off the vaginal canal as though there is a “wall“ there, not an opening. Pain doesn’t occur except when penetration is attempted. A girl’s first attempt at tampon insertion is excruciating—and often the first sign of a problem.
Vulvodynia is typically felt as burning or itch that can spontaneously appear or be provoked by tight clothing, sexual activity, a gynecological exam—or even sitting and walking! In both conditions, sexual intercourse becomes unbearably painful, if not impossible. Relationships suffer, and women often find themselves in a free-fall that can include depression, loneliness, self-loathing, and helplessness—especially if the pain persists for a very long time.

For women with vulvovaginal pain, “normal” things like tight clothing can be a big very deal.
Prevalence is difficult to determine partly because the conditions often overlap and studies require stressful gynecological exams, which tend to be avoided. Vulvodynia is said to be highly prevalent with lifetime estimates ranging from 10% to 28% in reproductive-aged women in the general population. The prevalence rates for vaginismus vary between 0.4 and 6.0% in the general population. Vaginismus rates are much higher in sexually conservative cultures.
Causes of Vulvovaginal Pain
In the not-so-distant past, vulvovaginal pain conditions were considered to be sexual neurosis, but that’s no longer the case.
That’s not to say there aren’t psychological contributors. There are, particularly with vaginismus. Both conditions, however, are bonafide health care issues that can respond well to treatment by a professional, or with self-treatment.
This pain certainly isn’t “all in your head,” but, surprisingly, many physicians—and even gynecologists—have never heard of these conditions. As recently as 2011, 80% of junior gynecologists in the UK had not attended a single educational session or training course on vulvodynia by the end of their specialty training. Research has only just started to trickle down to the medical textbooks in the last decade.
Vulvodynia research dominates sexual pain research, so more is known about it. Different subtypes exist (e.g., provoked vestibulodynia) and it’s best to consult a urologist or gynaecologist who understands the conditions. (They can be hard to find, so don’t give up too soon!) Physical causes and related conditions, like endometriosis and PCOS, need to be ruled out. Factors involved in vulvodynia can also include hormones, nerve density or trauma, genetics, inflammation, etc.
Less is known about vaginismus. Recent research has called into question whether the spasm exists as has been historically described (there is, in fact, no evidence of such muscle changes)—but it almost doesn’t matter for treatment.
The most effective treatments directly address your thoughts around the pain—how you think about and respond to the condition. Fear of penetration pain understandably makes you avoid any activity that can trigger pain, but by avoiding penetration, you never have a chance to gently confront your fears. It’s a never-ending reinforcing loop!
To be clear, the “fear” in vaginismus isn’t exactly your average fear. It has a phobic quality to it. Overcoming this fear is looking more and more likely to be the key to successful treatment. Working directly on pelvic floor muscle tension is secondary but still an incredibly useful treatment strategy.
Starting Pelvic Floor Physiotherapy Treatment for Vaginal Pain
One of the best treatments for vaginismus (and some types of vulvodynia*) is pelvic floor physiotherapy—which focuses on the muscles, skin, connective tissues in and around the pelvic region.
Because panic and fear are hallmarks of vaginismus, pelvic floor physiotherapists necessarily need to identify, understand and be sensitive to the needs of people with this kind of pain.
Pelvic floor physiotherapy helps you deal directly with negative penetration thoughts and associated anxiety by tackling those dreaded, automatic defensive reactions: the involuntary shaking, the legs clamping shut, the scooting away from touch, and so on. You deepen your awareness and control over your muscles—and your life!—by learning more about the many things that can cause or prolong a pain state.
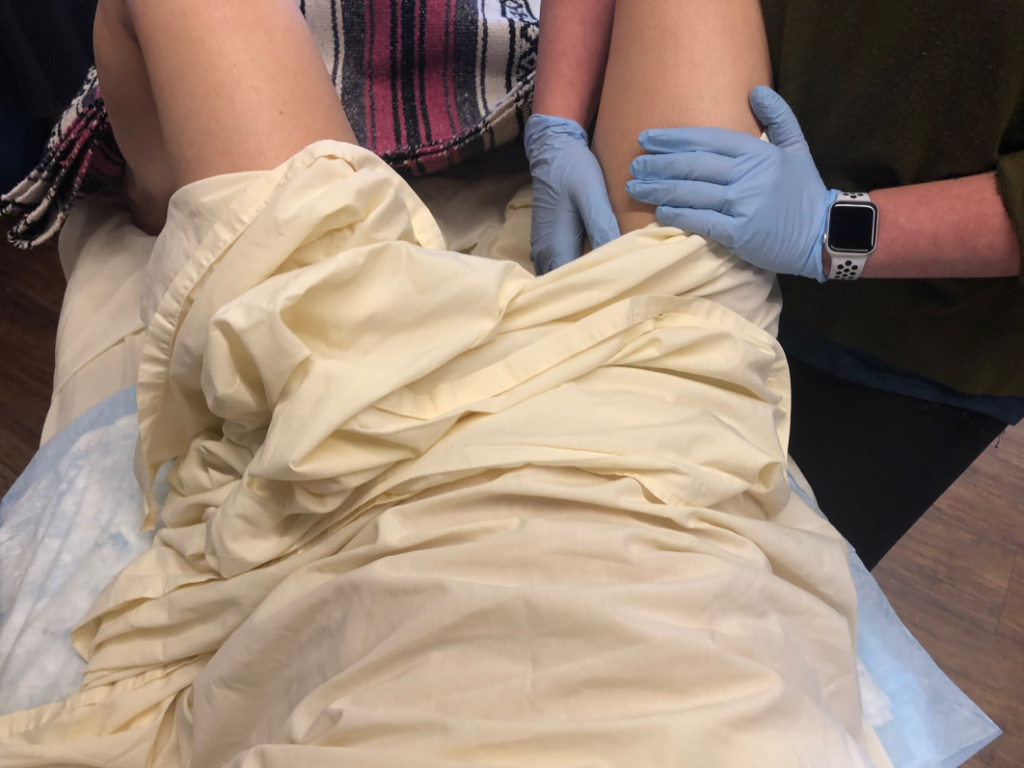
Although a typical pelvic floor session might include gentle internal work performed by a gloved physiotherapist, there’s no need to rush into it. Treatment often starts with a few sessions of external massage of the torso, hips, and legs while you and your therapist calm your nervous system and build therapeutic trust.
If you feel sickened or hesitant at the thought of pelvic floor physiotherapy, know you’re not alone—most sufferers don’t like the idea of it. You don’t need to be examined on the first visit if you don’t want to.
It’s a brave and positive move to simply reach out to a women’s health physiotherapist to see if you can talk with them. Baby steps count in vaginismus as you dismantle your long-held fear patterns. Consider contacting a few therapists to ask questions, compare notes and find one that you’re comfortable with.
If you cannot find or afford physiotherapy in your area, home vaginal dilation is an option. You can order sets of dilators online and find tips and techniques in the many online forums that exist for vulvovaginal pain. However, home dilation on its own does not address the emotional and cognitive aspects of the condition. You’ll have to do that for yourself. Find psychotherapeutic help if you can—especially with a practitioner well versed in phobic-like reactions. Even if they’ve never heard of vaginismus, they’ll understand the cognitive-behavioural aspects of it.
If you’d like to address some of your own cognitive-emotional factors, you’ll need to identify them first. If we know anything about vaginismus, it is that each person’s rendition is as unique as a fingerprint. You can download a Home Dilation Diary Plan for a research-backed way to gain self-insight into your particular mix of psychosocial factors with respect to vaginal penetration—then make more confident decisions about how and where to seek further help.
*Calming the nerves and reducing pelvic muscle tension (from guarding against pain) can often help immensely for vulvodynia, too.
PART 2 COMING SOON: “Pelvic Pain and Your Sensitive Nervous System”.
Learn More
Visit Vaginismus.com for relatable stories and information on diagnosis and treatment
Find a community of people with vaginismus at The Vaginismus Network
Visit the National Vulvodynia Association, the first organization formed to is to help improve the health and quality of life of women suffering from vulvodynia and chronic vulva pain without an identifiable cause.
Learn how to coordinate your breath with your pelvic muscles to create suppleness in your pelvic floor at Pelvienne Wellness.
Learn more about women’s sexual health at the International Society for the Study of Women’s Sexual Health
Visit the Vulval Pain Society for information for people with vulval pain and their partners
Kirsten Loop is a writer and designer living in Waterloo, Ontario, Canada. She is exploring a reconceptualization of vaginismus in her upcoming book merging pain science and lived experience. Her book is both informed and inspired by living with pelvic pain, and curing it as a young woman. Connect with her on Twitter, Instagram, Facebook, or reach out to her at the Edge of the Tribe.



 A Perfectionist’s Guide to Pain and Pacing
A Perfectionist’s Guide to Pain and Pacing